Heart Health & Preventive Cardiology
Ischaemic Heart Disease Singapore: A Silent Killer
By Dr Benji Lim, Senior Interventional Cardiologist, Novena Heart Centre

Heart attack
Did you know that ischaemic heart disease often strikes without warning? It also remains underdiagnosed, especially among high-risk groups.
In Singapore, this silent killer is the third leading cause of death after cancer and pneumonia. The Ministry of Health reported about 5,300 deaths in 2023, accounting for around 20% of all deaths.
Heart attack cases have also increased significantly. The number rose by about 44%, from 9,124 cases in 2012 to 13,137 in 2022. Alarmingly, nearly 1 in 7 patients had no symptoms at all.
What is IHD?
Coronary artery disease develops when plaque builds up in the arteries that supply blood to the heart. This plaque contains fat, cholesterol, and other substances. Over time, it narrows or blocks the arteries.
When this narrowing reduces blood flow to the heart, doctors diagnose ischaemic heart disease (IHD).
During physical activity, the heart needs more oxygen, so reduced blood flow becomes easier to notice and symptoms may appear. A ruptured plaque can form a clot and suddenly block the artery, which may damage the heart muscle and lead to a heart attack.
Symptoms of IHD
Angina is the most common symptom and occurs when reduced blood flow affects the heart. It causes chest pain or discomfort.
The pain may spread to the shoulder, arm, back, neck, or jaw. It often appears during physical activity, after meals, or during emotional stress, and usually lasts only a few minutes. Most episodes improve with rest or medication.
For some people, however, a heart attack may be the first sign of IHD.
A heart attack causes severe and persistent chest pain, often described as crushing, squeezing, or tight. The pain usually lasts more than 10–15 minutes and does not improve with rest. Without prompt treatment, permanent damage or sudden death may occur. People may also experience shortness of breath, sweating, nausea, or vomiting.
Older adults, women, and people with diabetes may show unusual symptoms. These can include fatigue, indigestion-like discomfort, back or jaw pain, dizziness, or fainting. Some people may not have any symptoms at all.
Because symptoms vary widely, early screening helps. Regular medical check-ups are also important. Overall, symptoms can differ from person to person.
Risk Factors for IHD
IHD, together with stroke and peripheral vascular disease, includes a wide range of conditions called atherosclerotic cardiovascular disease (ASCVD). Established risk factors for ASCVD can be grouped into modifiable and non-modifiable categories. Non-modifiable risk factors include:
• Age: Risk increases with age, especially in men over 45 and women over 55 years of age.
• Sex: Men are 3-5 times more likely to have IHD than pre-menopausal women, though women’s risk gradually equalises post-menopause.
• Ethnicity: In Singapore, Indians are more likely to have IHD, followed by Malays and then Chinese.
• Family history of premature IHD: Defined as under 55 in male relatives and under 65 years of age in female relatives.
• Genetic factors: These include inherited lipid disorders, such as familial hypercholesterolaemia.
Modifiable risk factors can be addressed through lifestyle changes and/or medical treatment. These include:
• Smoking: One of the strongest modifiable risk factors.
• Hypertension (high blood pressure)
• Hyperlipidaemia (high cholesterol)
• Diabetes mellitus (elevated blood sugar levels)
• Obesity
• Physical inactivity
• Unhealthy diets: Such as those high in saturated fat, trans fats, salt and refined sugars.
• Excessive alcohol consumption: Especially binge drinking or chronic excessive intake
• Psychosocial factors: Including chronic stress, depression and social isolation
Emerging risk factors also include lipoprotein(a), or Lp(a). It is a genetically determined particle that is similar to LDL (“bad cholesterol”) but contains an extra protein called apolipoprotein(a). High Lp(a) levels increase the risk of heart disease, stroke, and aortic valve disease.
What You Should Do
If you think you may have symptoms of IHD, do not ignore them. Your body may be warning you that something is wrong.
Seek medical attention promptly. If symptoms are severe, go to the nearest emergency department. Otherwise, arrange an early appointment with a cardiologist.
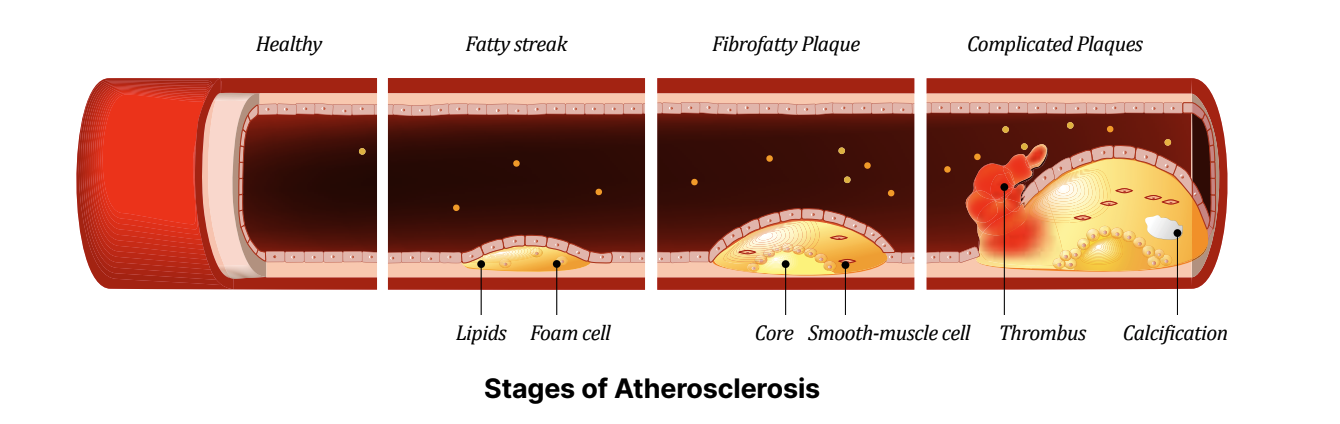
Stages of Atherosclerosis Dr Benji Lim
Diagnosis of IHD
For diagnosis, a cardiologist will review your symptoms and assess your heart risk profile. Depending on your condition, your doctor may recommend further investigations, such as blood tests, an electrocardiogram (ECG – a recording of the heart’s electrical activity), a treadmill exercise test, an echocardiogram (ultrasound scan of the heart that assesses its pumping function and condition of its valves), or a CT scan of the heart’s coronary arteries. While these non-invasive methods can detect IHD, they each have their own limitations and may occasionally yield false positives or negatives. In some clinical scenarios, or if non-invasive tests show significant blockages, an invasive coronary angiogram may be required.
Coronary Angiogram
A coronary angiogram is a minimally invasive procedure performed under local anaesthesia through a small incision in the wrist or groin. Doctors pass a thin, flexible tube (catheter) through the artery and guide it to the heart, where contrast dye is injected into the coronary arteries. Doctors take a series of X-ray images as the contrast flows through the arteries, revealing any blockages. A diagnostic coronary angiogram typically takes less than 30 minutes to complete. Based on the results of the diagnostic coronary angiogram, doctors can choose from three main treatment options. Depending on the severity and location of the blockages, treatment can include:
Conservative management:
For minor blockages or blockages in small arteries, medications such as blood thinners and cholesterol-lowering drugs may be sufficient.
Percutaneous coronary intervention (PCI): For severe blockages that are suitable, doctors may recommend PCI. This involves passing a thin guidewire through the blockage, delivering a balloon along the guidewire, inflating the balloon to open the blockage (angioplasty), and often subsequently placing a stent to keep it open. PCI usually takes 30-120 minutes, depending on complexity.
Coronary artery bypass grafting (CABG): Recommended for complex or multiple blockages (especially in diabetics). CABG is a surgical operation. Surgeons graft a healthy blood vessel (usually from the chest, leg, or arm) to a coronary artery beyond the blocked segment to restore blood flow to the heart muscle.
In some cases, or when intermediate blockages are detected, further evaluation with coronary physiology tests (e.g. pressure wire assessment) or intra-coronary imaging may help to determine the best course of action.
PCI – Balloon Angioplasty and Stenting
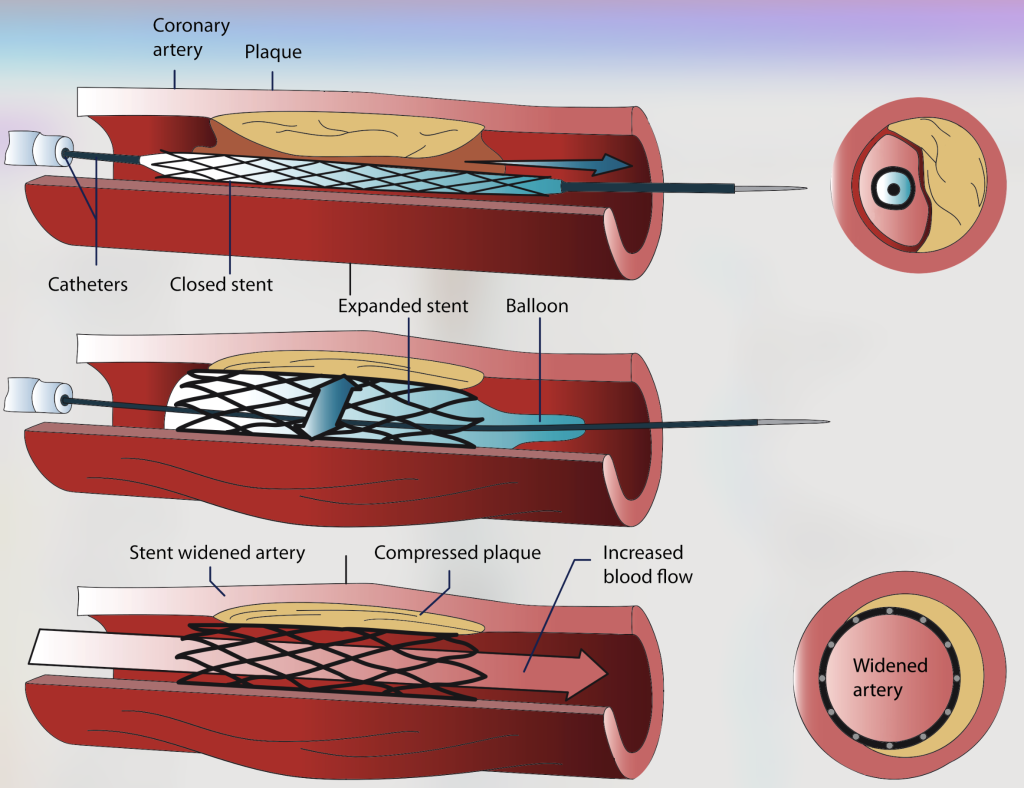
Angioplasty steps
Possible Recurrence
You may think, “If I had a severe blockage that was treated with angioplasty and stenting, I have nothing to worry about now, right?” Well, not quite. While angioplasty and stenting can greatly relieve symptoms and improve quality of life, recurrence is possible if risk factors are not controlled. Recurrence may involve re-narrowing of previously treated areas, or progression of previously minor blockages. Strict adherence to prescribed medications is critical. These medications often include blood thinners (e.g. aspirin, clopidogrel, ticagrelor) and cholesterol-lowering drugs (e.g. statins). Blood thinners reduce the risk of clot formation around stents and the treated segment of the artery – these, if they occur, can lead to a life-threatening heart attack.
Statins have also been proven to reduce cardiac risk by lowering LDL and stabilising cholesterol plaques in the arteries. Lifestyle modifications are equally essential: eat a heart-healthy diet, exercise regularly, quit smoking, and manage conditions such as hypertension, hyperlipidaemia and diabetes aggressively.
Conclusion
IHD remains a leading cause of death and disability in Singapore and globally. Fortunately, it is also one of the most preventable. With regular cardiac health screenings, early detection, lifestyle changes and timely medical interventions, people can greatly lower their risk. Through increased awareness and proactive care, many can continue to lead active, healthy and fulfilling lives. If you have risk factors or symptoms, speak to your doctor today about a heart health check. PRIME












Leave A Comment