Pain Management & Nerve Health
Burning or Tingling Pain? Understanding Neuropathic Pain Beyond Diabetes
by Dr Nivan Loganathan, Total Pain Specialist Clinic
What Makes Nerve Pain Different?
Pain is something most of us understand instinctively. When we twist an ankle, strain a muscle, or develop arthritis, the discomfort usually makes sense—it occurs where injury or inflammation happens.
Nerve pain, however, feels very different.
Neuropathic pain can:
- Burn or sting
- Tingle or numb
- Feel like electric shocks
Some people also develop extreme sensitivity to touch or temperature. In certain cases, pain appears without any obvious injury. This makes nerve pain confusing and frustrating for many patients.
Neuropathic Pain: Not Just About Diabetes
Many people associate neuropathic pain with diabetes. While diabetes is a common cause, it is not the only one.
In clinical practice, many patients develop nerve pain unrelated to blood sugar levels. These patients often spend months—or even years—searching for answers.
What Causes Neuropathic Pain?
Neuropathic pain develops when the nervous system itself becomes damaged or disrupted.
This may involve:
- Peripheral nerves in the arms and legs
- The spinal cord
- The brain
Unlike muscle or joint pain, nerve pain does not respond well to rest or anti-inflammatory medication. It often behaves unpredictably—flaring at night, worsening with stress, or persisting long after an injury heals.
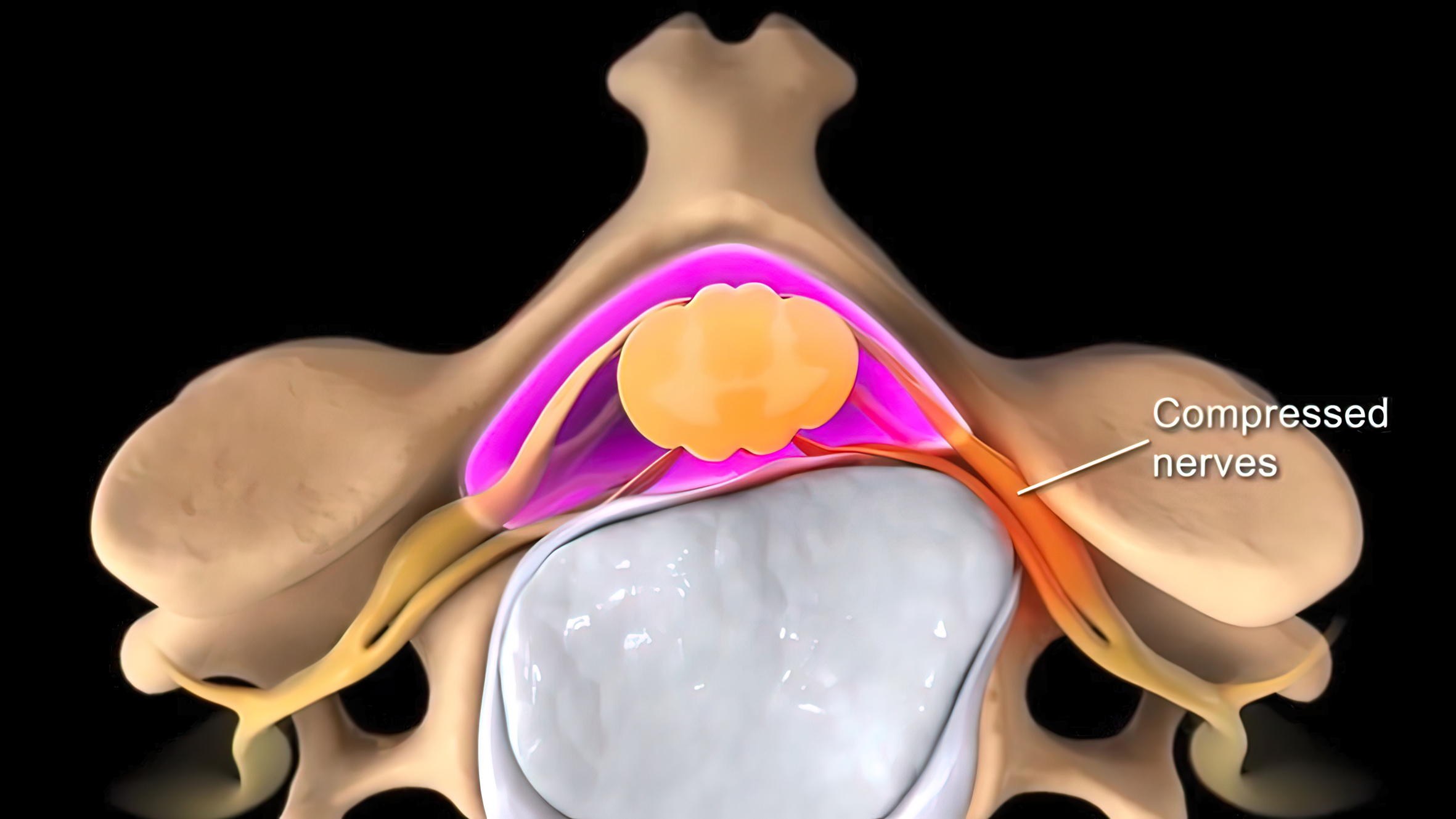
Spinal Nerve Compression from Herniated Disc Illustration
Why Nerve Pain Is Often Misunderstood
Nerve pain does not follow typical patterns, which makes it harder to recognise.
Patients may:
- Feel pain and numbness at the same time
- Experience pain from light touch (like clothing)
- Struggle to describe their symptoms clearly
Standard scans and blood tests may also appear normal. Because of this, doctors may underestimate the condition, especially when symptoms seem vague.
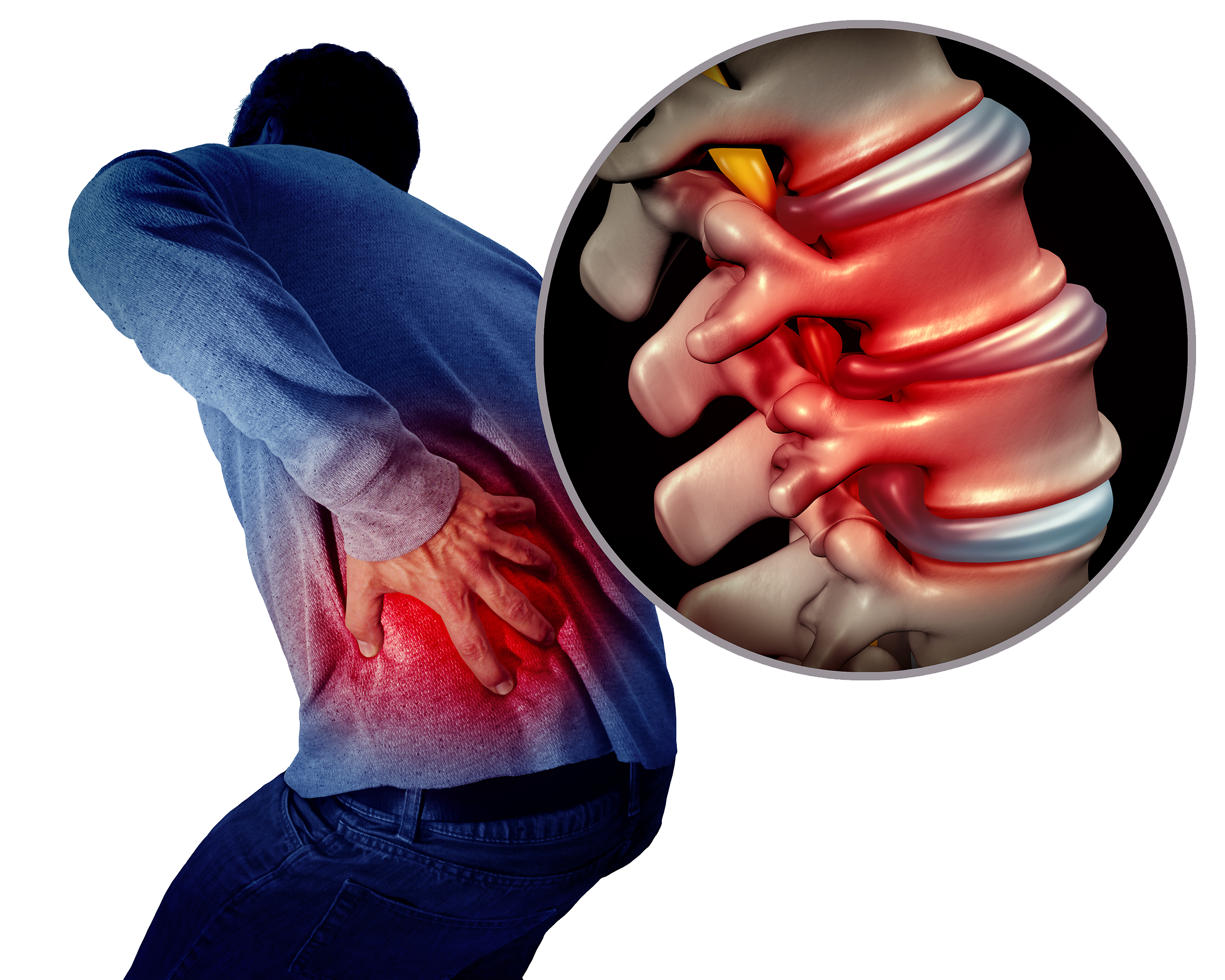
Sciatica Pain Caused by Nerve Compression in the Lower Spine
Common Causes Beyond Diabetes
Physical Injury and Trauma
Injuries such as car accidents, sports trauma, or falls can stretch or compress nerves. Even minor injuries may lead to long-term nerve pain.
Post-Surgical Nerve Pain
Most surgeries heal well, but in some cases, procedures may irritate or damage nearby nerves. This can lead to persistent pain after recovery.
Spinal Conditions
Conditions such as:
- Slipped discs
- Spinal stenosis
- Degenerative spine changes
can compress nerves and cause radiating pain (commonly known as sciatica). If untreated, this may lead to long-term nerve sensitisation.
Infections
Shingles is a well-known cause of nerve pain. Even after the rash disappears, some patients develop long-lasting burning pain known as post-herpetic neuralgia.
Nutritional and Metabolic Causes
Low levels of vitamin B12 can affect nerve function. Toxins such as alcohol or chemotherapy drugs may also damage nerves over time.

Physical Therapy Treatment for Knee and Nerve-Related Pain
Why Early Diagnosis Matters
If doctors do not recognise neuropathic pain early, it can become chronic.
Repeated irritation can make nerves overactive. They may continue sending pain signals even after the original problem resolves. This process is known as sensitisation.
Patients should seek medical advice if they experience:
- Persistent burning or tingling
- Shooting or electric-like pain
- Unexplained numbness
- Pain that does not improve with usual treatment
Early evaluation helps identify nerve involvement and prevents long-term complications.
How Doctors Diagnose Nerve Pain
Diagnosing neuropathic pain relies heavily on clinical assessment.
Doctors will:
- Take a detailed history of symptoms
- Perform a neurological examination
- Look for signs such as sensory changes or allodynia
They may also use:
- Blood tests
- Nerve conduction studies
- Imaging
These tests help rule out other conditions and confirm nerve involvement.
Treatment: Why It Requires a Different Approach
Nerve pain needs a different treatment strategy from typical pain.
Medications
Standard painkillers often do not work well. Instead, doctors prescribe medications that target nerve signals and calm overactive nerves.
Interventional Procedures
In some cases, targeted treatments such as:
- Nerve blocks
- Injections
- Minimally invasive procedures
can reduce inflammation and interrupt pain signals.
Advanced therapies like neuromodulation may help patients with persistent symptoms.
The Role of Lifestyle and Mental Health
The nervous system closely connects with emotional and physical well-being.
Factors that can worsen pain include:
- Poor sleep
- Stress
- Anxiety
Managing these factors improves outcomes. Good sleep, gradual activity, and stress management all support recovery.
Rehabilitation and Recovery
Movement plays an important role in recovery.
Physiotherapy and guided exercise:
- Help retrain the nervous system
- Improve mobility
- Restore confidence
Contrary to common fears, appropriate movement does not worsen nerve damage. It often supports healing.
Nerve Pain Is Real — And Treatable
Many patients feel isolated or dismissed when dealing with nerve pain. Some believe their symptoms are psychological or untreatable.
This is not true.
Neuropathic pain is a real medical condition. With early diagnosis and a personalised treatment plan, patients can achieve meaningful improvement.
Understanding the condition is the first step. With the right care, nerve pain does not have to define a person’s life. PRIME












Leave A Comment