Mr Chan is a middle-aged man with chronic hepatitis B. He had regular follow-ups at his neighbourhood polyclinic. However, doctors later referred him for further checks after an ultrasound suggested liver scarring.
When Mr Chan first saw me, he felt very worried. This is because his friends had told him that liver scarring—also called liver fibrosis—is irreversible and life-limiting. However, I reassured him. While liver fibrosis is serious, doctors can slow or even stop its progression. More importantly, early diagnosis and treatment can make a big difference.
LIVER FIBROSIS AND CIRRHOSIS
Liver fibrosis refers to scar tissue that forms after liver injury. When the liver is damaged, it sends signals to activate repair cells. As a result, these cells produce substances such as collagen, a type of fibre.
Over time, repeated injury causes collagen to build up in the liver. Consequently, scar tissue forms and the liver becomes stiff. In addition, this scar tissue reduces blood flow and affects healthy liver cells. As the condition worsens, the liver becomes irregular and nodular.
In general, fibrosis develops slowly over one to two decades. At first, it may remain mild. However, it can progress to advanced stages if left untreated. Eventually, it may develop into cirrhosis, which causes permanent and severe damage.
CAUSES AND SYMPTOMS
Common causes of liver fibrosis include:
-
Chronic hepatitis B and C
-
Non-alcoholic fatty liver disease (NAFLD)
-
Alcohol-related liver disease
In the early stages, most patients do not have symptoms. Therefore, many people are unaware of the condition. However, as cirrhosis develops, symptoms may appear.
For example, patients may experience:
-
Yellowing of the skin and eyes
-
Abdominal swelling
-
Vomiting blood or passing black stools
-
Easy bruising
-
Confusion or poor focus
-
Sleep problems
In addition, patients with cirrhosis have a higher risk of liver cancer.
ASSESSMENT
Doctors can assess liver fibrosis using non-invasive tests. These include blood tests and imaging scans.
For instance, common tools include:
-
Fibroscan (transient elastography)
-
Magnetic resonance elastography (MRE)
A Fibroscan measures liver stiffness using sound waves. In general, stiffer liver tissue suggests more scarring.
Besides that, doctors also use blood test scores such as:
-
NAFLD Fibrosis Score (NFS)
-
Fibrosis-4 (FIB-4) score
These scores help rule out advanced fibrosis.
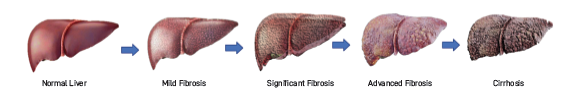
Fibrosis is graded from F0 to F4:
-
F0: No fibrosis
-
F1: Mild fibrosis
-
F2: Moderate fibrosis
-
F3: Severe fibrosis
-
F4: Cirrhosis
However, liver biopsy remains the gold standard. During this test, doctors take a small tissue sample for closer examination. As a result, they can assess the level of inflammation and scarring.
Overall, assessing fibrosis helps guide treatment. It also helps predict outcomes. In general, higher stages carry higher risks.
In Mr Chan’s case, he had no symptoms. In addition, his physical exam was normal. However, blood tests and a Fibroscan showed stage 3 fibrosis.
TREATMENT
The best treatment targets the underlying cause.
For Mr Chan, we started antiviral medication for hepatitis B. We also advised lifestyle changes. He now follows a healthier diet and exercises regularly. He aims for at least 30 minutes of moderate activity, five times a week.
In early stages, treatment can reverse fibrosis. In later stages, treatment helps prevent complications.
Liver function may remain stable at first (compensated cirrhosis). Over time, it may worsen and lead to complications (decompensated cirrhosis). In severe cases, liver failure can occur.
When complications develop, care focuses on managing them. Doctors may also consider liver transplantation or palliative care, depending on the patient’s condition.
SURVEILLANCE and TREATMENT of COMPLICATIONS
Cirrhosis can lead to several complications:
-
Jaundice
-
Ascites (fluid in the abdomen)
-
Varices (enlarged veins in the oesophagus or stomach)
-
Encephalopathy (confusion and poor concentration)
-
Infections
-
Liver cancer
Patients with advanced fibrosis or cirrhosis need regular follow-up. Doctors usually review them every six months. These visits include symptom checks and blood tests.
Patients should also undergo liver ultrasound every six months. This helps detect early liver cancer.
Some patients may need an endoscopy (OGD) to check for varices. Doctors may treat varices with medication or banding if needed.
THE CASE OF MR CHAN
At the end of the consultation, Mr Chan felt more confident. He now understands his condition and how to manage it.
His case shows an important point. With early diagnosis and proper treatment, patients with liver fibrosis can live well and maintain a good quality of life. PRIME













Leave A Comment