
Haemorrhoids, commonly known as piles, are a very common condition in Singapore. Studies suggest that up to one in three people may experience this condition at some point in their lives. Many people feel embarrassed and delay seeing a doctor. They often seek medical attention only when bleeding, pain, or prolapse becomes significant enough to affect their quality of life.
In fact, haemorrhoids are normal structures that are present in everyone. They sit in the mid-anal canal and are commonly referred to as anal cushions. These cushions contain blood vessels and serve an important function in preserving continence.
In this article, I will address some of the most common myths surrounding piles and help readers gain a clearer understanding of the condition.
Myth 1: Haemorrhoids or piles are abnormal and should always be removed.
FALSE!
Haemorrhoids are a normal part of the anal canal. Together with the anal muscles, they form an essential part of the continence mechanism and help us hold in stool. Doctors should leave them alone if they do not cause symptoms.
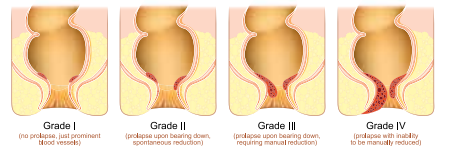
Treatment becomes necessary only when piles cause problems. Doctors refer to this as haemorrhoidal disease. Patients commonly present with fresh, bright red bleeding, pain, prolapse of enlarged piles, or a combination of these symptoms.
Myth 2: Haemorrhoids only affect older adults.
FALSE!
Piles can affect people of all ages. In my clinical experience, the most commonly affected age group is between 20 and 40 years old. This group makes up about 75% of my patients. However, the risk does increase with age. Women are also more likely to be affected, especially after pregnancy and childbirth.
Myth 3: If I am young, healthy, and exercise regularly, I should not get piles — especially if I eat plenty of fibre.
FALSE!
In recent years, I have observed a noticeable rise in the number of patients seeking treatment for piles. In my practice, this increase has been roughly 20% year on year over the past five years. Lifestyle factors appear to play a major role in this trend.
Lifestyle Factors That Increase the Risk of Piles
Dietary habits, toileting behaviour, and certain forms of exercise all influence the development of haemorrhoidal disease. Popular dietary trends, such as ketogenic diets and veganism, can significantly alter bowel habits and stool consistency. A lack of balance in the diet may lead to problems at either end of the spectrum.
In my practice, many patients with constipation consume excessive fibre without adequate hydration. These individuals often experience bloating, flatulence, and pellet-like or bulky stools, corresponding to Bristol Stool Chart types 1 and 2.
Prolonged and excessive straining further worsens the problem. Spending too much time on the toilet bowl also increases pressure on haemorrhoidal tissue, and mobile phones and tablets often contribute to this habit. Certain exercises, such as heavy weightlifting, add further strain by increasing intra-abdominal pressure. Together, these factors explain why more young adults are developing haemorrhoidal disease.
.
Myth 4: Exercising more intensely and taking more fibre will reduce my risk, as long as I pass stool daily.
FALSE!
Repetitive and prolonged exercises that involve significant straining, such as weightlifting and squatting, can cause haemorrhoidal tissue to swell excessively. This effect becomes more pronounced when combined with other lifestyle factors. These include an unbalanced diet and prolonged time spent on the toilet bowl.
Many people believe they must pass stool every day. This misconception leads them to sit and strain on the toilet unnecessarily. Sitting on the toilet bowl causes haemorrhoidal tissue to swell. This swelling is reversible and not harmful if a person limits toilet time to five to ten minutes.
Myth 6: Bleeding from the bottom is always caused by piles.
FALSE!
Although piles commonly cause rectal bleeding, other conditions can also be responsible. Some of these conditions are serious, including colorectal cancer (CRC). This concern is particularly important in Singapore, where CRC is the most common cancer in men and the second most common in women.
Doctors are also diagnosing CRC more frequently in younger individuals. Up to one in five people diagnosed with CRC are now below the age of 50. You should never assume that rectal bleeding is due to piles alone.
Seek medical attention promptly if bleeding occurs alongside symptoms such as pallor, fatigue, weakness, or unexplained weight or appetite loss.
I recommend screening colonoscopy from the age of 45 for individuals without symptoms. Those with symptoms or a family history of CRC should undergo screening earlier. In cases with a family history, screening should begin ten years before the age at which the first affected relative was diagnosed.
Early detection makes a significant difference. Removing pre-cancerous polyps during colonoscopy can prevent CRC, and early-stage cancers often respond very well to treatment. However, many early cases do not cause pain, bleeding, or weight loss. These symptoms more commonly appear in advanced disease.
Myth 7: Probiotics are not useful for piles.
FALSE!
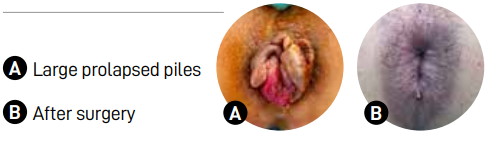
The management of piles focuses on correcting lifestyle triggers, optimising diet and toileting habits, and using medications when needed. Surgery remains a last resort.
Probiotics can serve as a useful adjunct. By helping to regulate stool consistency, they support the formation of type 4 stools, which resemble bananas or sausages. These stools pass through the anal canal more easily and place less strain on haemorrhoidal tissue.
Regular probiotic use may also support gut health and reduce episodes of diarrhoea. Diarrhoea can cause haemorrhoids to swell and trigger symptoms. By improving stool consistency, probiotics help lower this risk.
Final note from the doctor
Piles are common, treatable, and often preventable. Early attention to symptoms, combined with balanced lifestyle choices and timely medical advice, can prevent unnecessary discomfort and complications. PRIME














Leave A Comment