Eye Health Series
Understanding More about Cataract
by Dr Jayant V Iyer – The Straits Eye Centre
Cataract is the leading cause of blindness and vision impairment worldwide. Nearly 100 million people globally have poor eyesight because of this condition. In Singapore, one in three adults over the age of 40, and four in five adults over the age of 65, have this condition. Yet, many of us may not fully understand this condition, including its causes, symptoms, diagnosis and treatment. Let us now take a closer look at cataract and find out more about this common ailment, especially in terms of treatment.
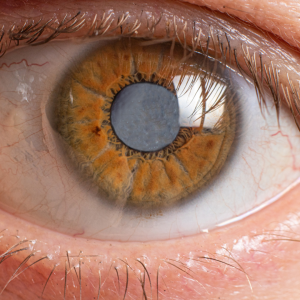
lens options for cataract treatment in Singapore
CAUSES AND SYMPTOMS
Just like a camera, every eye has a lens inside that allows us to focus and see clearly. As we get older, this natural transparent lens becomes foggier. This condition is known as cataract.
Ageing is the most common cause of cataract. Singapore has an ageing population, so we are seeing an increasing number of people with cataracts in our country. Other causes of cataract include chronic use of steroid medications, injury to the eye and genetics.
In its early stages, cataracts may be present without any symptoms. If you have an early cataract that does not affect your day-to-day function, you do not need to worry about it. Nothing needs to be done! However, sometimes, cataract may cause your degree to fluctuate, and you may need to change your spectacles. Other common symptoms include dimmer vision, haloes, glare and persistently poorer vision. When cataract affects your vision and day-to-day life, it will need to be treated.
DIAGNOSIS
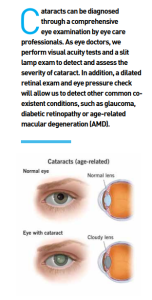
Cataracts can be diagnosed through a comprehensive eye examination by eye care professionals. As eye doctors, we perform visual acuity tests and a slit lamp exam to detect and assess the severity of cataract. In addition, a dilated retinal exam and eye pressure check will allow us to detect other common co-existent conditions, such as glaucoma, diabetic retinopathy or age-related macular degeneration (AMD).
Comparing an eye to a camera might make this a little easier to understand. You can liken a cataract to a faulty lens in the camera – just replacing the lens may restore its function. However, a camera with other problems, such as those involving other parts of the mechanism or memory card may require different solutions, just as an eye with glaucoma or retinopathy may require other treatment options.
You may then ask: but can we prevent cataract? Well, just do not grow old! As we know, this is not yet entirely possible. However, there are certain measures you can take to reduce the severity of cataract or delay its development. These measures include wearing sunglasses with ultraviolet protection, quitting smoking, eating a diet rich in antioxidants, and optimally managing other systemic conditions one may have, such as diabetes mellitus.
TREATMENT
In its early stages, just changing glasses or contact lenses may be adequate to optimise vision. In later stages or in situations where the quality of vision is significantly bad despite being able to see with glasses, cataract surgery is the only real solution.
As a result of the above, there are some people who seem to believe that they need to go for cataract surgery only when the cataract is “ripe”. This is not true. Three to four decades ago, this may have been the case when we had older surgical techniques with a significant complication rate. In recent times, cataract surgeries have become much safer and less invasive. Success rates are much higher and complication rates are significantly lower in less severe cataracts. As such, it is, in fact, advisable to consider cataract surgery, in consultation with your ophthalmologist, the moment it starts affecting your day-to-day function.
CATARACT SURGERY
Cataract surgery was first described in ancient India by the physician Sushruta over 2,000 years ago. The technique known as “couching” involved inserting a heated metal rod to push the dense cataract into the back of the eye. This restored some vision but was fraught with complications.
Modern techniques are far safer and more effective in restoring vision. Cataract surgery is currently one of the most commonly performed surgeries worldwide. At The Straits Eye Centre, our success rates are in excess of 98% to help our patients achieve clearer, brighter and better vision. Our complication rates are below 1%.
Modern cataract surgery involves making a 2mm incision on the eye. We then use a “phacoemulsification” machine to fragment the cataract into tiny pieces and extract it from the eye. Over the last few years, some surgeons use the assistance of femtosecond laser for even greater precision and added safety.
Following this, we then insert a clear artificial lens into the eye to restore vision. We work as a team with our anaesthetist to keep our patients comfortable and relaxed with gentle sedation. We also use anaesthetic eyedrops to ensure the patient feels no pain throughout the surgery. The procedure typically lasts 10-15 minutes and the patient goes home the same day. As the incision is so tiny, it will usually heal well on its own without any stitches.
ARTIFICIAL LENS OPTIONS
There are many types of artificial intraocular lens implants (IOL) available for use: monofocal, extended depth of focus (EDOF), multifocal and toric lenses.
The most commonly used lens implants are monofocal IOLs. These lenses allow for crisp and clear vision for a particular distance range. Typically, most patients and surgeons opt for emmetropia. Patients are able to get crisp, clear and bright distance vision, but would need to use reading glasses for near and intermediate distance. Some patients with very high astigmatism may benefit from toric lenses to reduce the need for spectacle correction following the operation.
For patients who would like to be spectacle-independent as much as possible, EDOF lenses and multifocal lenses provide a good option in allowing for reasonably good vision for various distance ranges – near, intermediate and far. However, these premium IOLs are more expensive and come with some additional side effects, including increased glare, reduced contrast and night-time haloes. Certain patients, including those with concomitant conditions such as glaucoma or high myopia, may not be best suited for this option. Hence, if you have a visually significant cataract, please discuss these options with your surgeon.
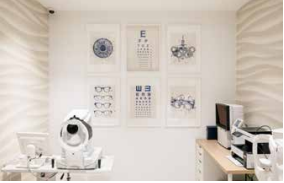
cataract treatment Singapore – eye examination
RISKS AND RECOVERY
Cataract surgery is one of the safest operations in the world, especially when performed by senior surgeons. However, even in the best hands, there can be complications. 1-2% of patients may get complications, such as retinal detachment, poor wound healing and prolonged inflammation. Very rarely may the cataract drop into the eye during surgery; this would require another corrective surgery. Even more rarely, about one in one thousand patients may go blind from the surgery due to severe infection. Thankfully, such complications are uncommon. It is important to discuss the potential risks and benefits of cataract surgery with your eye care professional.
Recovery time may vary from person to person following cataract surgery. Most patients may expect good vision within a month, although some patients achieve this even sooner!
While patients are entitled to one month of hospitalisation leave following cataract surgery, many of my patients choose to return safely to work one week following the operation.
During the first post-operative week following surgery, we advise our patients to not engage in any vigorous physical activity and advise that they do not rub their eye(s) or allow water to get into their eye(s). We also prescribe them a one-month course of antibiotics and steroid eyedrops to help with the healing process and prevent infections.
CAN CATARACTS COME BACK AFTER SURGERY?
Once the clouded lens is removed during cataract surgery, it cannot develop a cataract again. However, in 10-20% of patients, a condition called posterior capsular opacification may occur after some time following the surgery. This condition may result in hazy vision and happens when some cells form a layer behind the artificial lens implant – much like dust on a windowpane. This condition can be easily treated with a laser procedure called a YAG capsulotomy, and most patients regain their clear vision within a day or two following the procedure.
TAKE-HOME MESSAGE
It is always good to go for general eye screening if you are above the age of 40, have high myopia, or have a family history of conditions such as glaucoma and retinal detachment. If you are diagnosed with cataract, do not worry. This is an extremely common condition. And if the cataract is indeed affecting your vision and quality of life, current treatment options are extremely safe and effective in helping to restore your vision. It is best to seek the guidance of an eye doctor. PRIME













Leave A Comment